Pennsylvania Insurance Commissioner Teresa Miller is reminding health insurers that they must keep their provider directories up to date and that consumers should not pay higher out-of-network costs if they use a health care provider who is out-of-network but, at the time the service was provided, was listed in their insurer’s provider directory as in-network.
Miller said Monday that Gov. Tom Wolf’s administration is working to ensure that consumers are protected from common unfair insurance practices. “Since it is the insurers’ responsibility to keep their provider directories up to date, my department will use its authority under the Unfair Insurance Practices Act to see that consumers who do their homework to make sure that the doctors and hospitals they are using are in their insurance network will not suffer financial harm just because those directories are out of date,” the commissioner said.
Miller noted that Pennsylvania law prohibits unfair or deceptive acts or practices by insurers, including publishing or circulating an advertisement, announcement, or statement which is untrue, deceptive, or misleading. She said that if a person receives health care services from a provider listed in the insurer’s provider directory as in-network, and the insurer then attempts to settle that claim as if the provider were out-of-network, her department will consider this to be an unfair claim settlement practice.
“The provider directory must be a source on which consumers can rely for critical health care information,” said Miller. “We have received complaints from people who have undergone major medical procedures, thinking the doctors and hospitals they used were in-network, only to receive surprise bills of hundreds or even thousands of dollars.”
Miller reminded insurers that since open enrollment begins for many health plans on Nov. 1, now is a good time to ensure their provider directories are up to date. The Insurance Department said it will examine the overall issue of surprise balance billing at a public hearing on Oct. 1 in Harrisburg, Pennsylvania.
Miller advises that any Pennsylvania consumer who receives health care services from providers listed in their insurer’s directory as in-network when the services were provided, and are later told one or more of these providers was out-of-network, should contact their insurance company. She said if the insurer does not agree to cover these services at in-network rates, the consumer should contact the Insurance Department.
Source: The Pennsylvania Insurance Department
Topics Carriers Pennsylvania
Was this article valuable?
Here are more articles you may enjoy.


 USI Insurance Services Claims Ex-Broker Poached Clients for Own New Agency
USI Insurance Services Claims Ex-Broker Poached Clients for Own New Agency  Roof Costs Soar Even as Claims Decline: Verisk
Roof Costs Soar Even as Claims Decline: Verisk 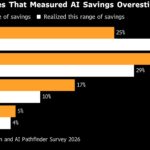 AI Savings Misses ‘Should Be Making Executives Uncomfortable,’ Bain Says
AI Savings Misses ‘Should Be Making Executives Uncomfortable,’ Bain Says  Florida’s Property Tax Plan Risks Charging Fees for ‘Everything’
Florida’s Property Tax Plan Risks Charging Fees for ‘Everything’ 

