Delaware Insurance Commissioner Karen Weldin Stewart announced that insurers will issue more than $2 million in rebates to 14,399 health insurance policyholders in Delaware as a result of the Affordable Care Act’s 80/20 medical loss ratio rule.
The rule requires insurers in the individual and small group markets to spend at least 80 percent of premium dollars on medical costs and activities that improve the quality of health care, and no more than 20 percent on administrative costs, including executive salaries, overhead and marketing.
In the large group market, the ratio is higher — insurers must spend at least 85 percent of premiums on health care and quality improvements.
Any company selling health insurance in Delaware that fails to meet these standards will owe policyholders a refund. Rebates for individual market premiums are paid directly to the consumers, while those for small and large groups are paid to the employer who purchased those group plans.
Rebates may take the form of a check in the mail, a lump-sum reimbursement to a bank account (if the premium was paid by credit or debit card), or a direct reduction in future premiums.
The following chart provides a list of those insurers who owed rebates to Delaware consumers based on their medical loss ratio for coverage year 2014. Any company not listed equaled or exceeded the medical loss ratio requirement:
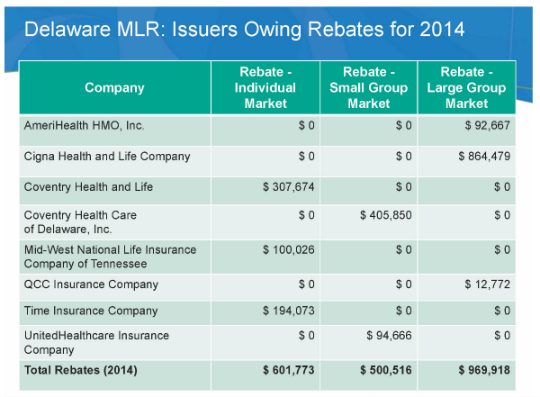
Source: The Delaware Department of Insurance
Topics Carriers
Was this article valuable?
Here are more articles you may enjoy.


 NY Lawmakers Agree to Governor’s Auto Insurance Reforms in New Budget
NY Lawmakers Agree to Governor’s Auto Insurance Reforms in New Budget  Georgia Brokers and Agents Alarmed After Court Ruling Expands Liability for Them
Georgia Brokers and Agents Alarmed After Court Ruling Expands Liability for Them  AI Savings Misses ‘Should Be Making Executives Uncomfortable,’ Bain Says
AI Savings Misses ‘Should Be Making Executives Uncomfortable,’ Bain Says  Warmer World Means Bigger Hail and More Damage, Study Finds
Warmer World Means Bigger Hail and More Damage, Study Finds 

