A small number of physicians are responsible for a large portion of the independent medical review of workers’ compensation cases in California, a process that could be costing payers in excess of $100 million, a report shows.
The IMR process was established by the state’s sweeping workers’ comp reform law, Senate Bill 863, which was passed in 2012.
The law was intended to save money and streamline the process for dealing with injured workers, but an unintended consequence was a large number of IMR requests that started flowing in after the law went into effect.
The high volume of IMR requests swamped the system at first, but much of the backlog has been worked through, according to the state’s Department of Worker’s Compensation.
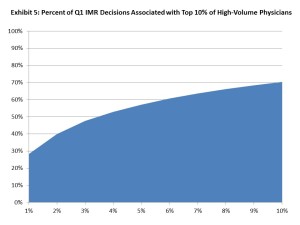
Source: California Workers’ Compensation Institute
However, the high volume of IMR letters has yet to subside, according to the study by the California Workers’ Compensation Institute.
The CWCI analysis issued in early July shows there was no significant reduction in IMR volume in the first quarter of this year. During that period, Maximus Federal Services, the independent medical review organization contracted by the state to manage California’s IMR process, issued a total of 33,909 IMR determination letters, the report shows.
The findings are not what lawmakers and proponents of SB 863 intended.
“Legislators who enacted IMR expected that the volume of applications would diminish following an initial learning curve as physicians, attorneys and others involved in the process would gain an understanding of the types of treatment that would meet the evidence-based medicine standards and be approved through (utilization review) and IMR,” the report states.
Since January 2014, there has been a steady stream of IMR applications, with the monthly totals averaging at 12,510 applications per month over the 15-month span studied, the report shows.
More telling is the report’s findings that out of the nearly 5,200 physicians associated with IMR disputes in the first three months of this year, the 10 percent with the highest volume of disputed requests were named in 70 percent of the IMR decision letters, while the top 1 percent accounted for 28 percent of the disputed requests that went through IMR.
“What we know from the data and from the research is that the requests are being submitted by a relatively small number of providers who seek a second opinion on a UR decision, which either modified or denied a treatment request,” said Alex Swedlow, CWCI’s president and chief executive officer.
He couldn’t say why such a small number of physicians accounted for most of the IMR requests – though he’s planning on a follow up study to look into that – but he noted that there is no expense for a provider to file an IMR appeal of a UR decision.
“Virtually all expenses associated with independent medical review are payed by the payer,” Swedlow said.
The average cost per review, according to Maximus, is now roughly $400, which doesn’t include other expenses the payer must cover.
“It’s estimated the overall costs of this process could be well over $100 million,” Swedlow said.
Sedlow, who does not advocate for policy, said those interested in dealing with this issue may seek to require a fee for the IMR process to reduce the volume, something similar to what is done in independent bill review process.
The report shows that prescription drugs topped the list of services submitted for IMR, accounting for 48 percent of the first quarter IMR decisions. Requests for prescription drugs, physical therapy, durable medical equipment, injections and diagnostic tests and measurements together accounted for three-fourths of all services submitted for IMR in the first quarter, according to the report.
A review of the IMR decisions issued in the first quarter shows that IMR physicians upheld the UR doctor’s modification or denial of the service 89 percent of the time, nearly matching the 91 percent uphold rate from 2014.
That shows the IMR and UR processes are working, Swedlow said.
“The process is running more efficiently, it’s just running at a very, very high volume,” he said.
Topics California Workers' Compensation
Was this article valuable?
Here are more articles you may enjoy.


 USI Insurance Services Claims Ex-Broker Poached Clients for Own New Agency
USI Insurance Services Claims Ex-Broker Poached Clients for Own New Agency  Florida Court Says 2020 Law Gives ‘Very Broad’ Liability Immunity to Rideshare Firms
Florida Court Says 2020 Law Gives ‘Very Broad’ Liability Immunity to Rideshare Firms  First Brands Hit by $286 Million Claim for Alleged Tariffs Fraud
First Brands Hit by $286 Million Claim for Alleged Tariffs Fraud  NY Archdiocese Can Depose Chubb CEO Greenberg in Clergy Abuse Claims Case
NY Archdiocese Can Depose Chubb CEO Greenberg in Clergy Abuse Claims Case 


